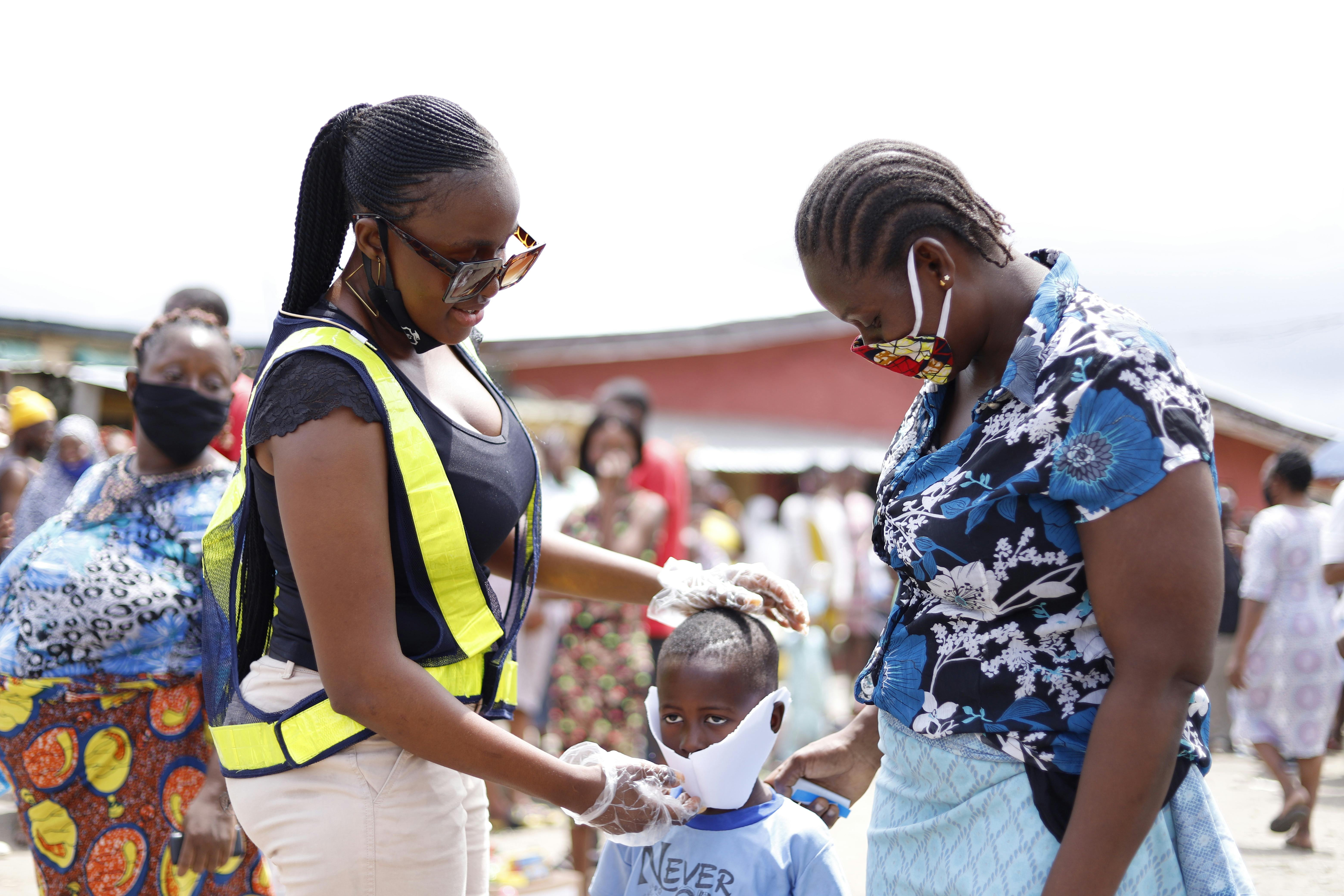Health
Maternal and Child Health Continuity Model: From Pregnancy to Early Childhood With Dignity
How a continuity-first maternal and child health model can reduce drop-off, improve outcomes, and preserve dignity from pregnancy through early childhood.
Maternal and Child Health Continuity Model
Kenford Trust approaches community health as a long-term systems challenge instead of a one-day event. In many underserved communities, people do not lack motivation to seek care; they lack predictable pathways that make prevention practical, affordable, and respectful. This article presents a field-informed framework for designing local health programs that can scale while preserving trust.
Our current objective focuses on continuous, respectful maternal and child health support from first antenatal contact through the child's early developmental milestones. To make this objective real, we combine outreach data, neighborhood leadership, facility collaboration, and follow-up discipline. The design principle is straightforward: if people are expected to adopt healthy behaviors, then services, information, and referrals must meet them where they are, in language they trust, at times they can realistically attend.
Across counties and mixed urban-rural settings, one pattern remains consistent. Programs succeed when teams treat prevention as a shared community function rather than a technical message delivered by experts alone. Community health volunteers, youth groups, teachers, caregivers, and facility staff each hold part of the solution. Coordination among these actors determines whether progress is temporary or durable.
Why Context Mapping Comes First
Before launching activities, teams should run a practical context mapping phase. This mapping documents who is missing routine care, why they are missing it, which care points are closest, what social barriers are strongest, and what local leaders already influence behavior. A strong map helps avoid generic campaigns that fail to address actual barriers.
Context mapping also helps teams identify hidden strengths. Some neighborhoods already have trusted parent groups, active faith leaders, or teacher mentors who can host health literacy sessions. By building on these existing structures, programs accelerate trust and reduce operational friction.
Most importantly, context mapping creates a baseline. Without a baseline, it is difficult to judge whether outreach is improving screening rates, referral completion, and continuity of care. Baseline clarity allows teams to improve implementation instead of relying on assumptions.
Community Realities Informing the Model
Expectant mothers frequently report that the first clinic visit feels manageable, but repeat visits become difficult as transport costs rise and family responsibilities increase. Continuity planning must therefore include social and economic realities from the beginning.
Community birth companions often understand household dynamics better than formal providers. When they are linked to facility teams through a clear referral protocol, women receive more consistent encouragement to complete antenatal pathways.
In many communities, fathers are willing to support maternal health but lack practical information. Structured father-inclusive sessions can transform passive support into concrete actions such as transport planning and postnatal monitoring.
Postnatal care is commonly misunderstood as optional when the delivery appears uncomplicated. Outreach messaging must explain why postpartum checks are essential for both mother and child, even in seemingly stable cases.
Caregivers of newborns often navigate conflicting advice from relatives, social media, and neighbors. Trusted local educators can reduce confusion by offering consistent guidance anchored in evidence and practical examples.
Nutrition counseling is more effective when linked to local food availability and household purchasing patterns. Generic recommendations rarely translate into action without adaptation to community context.
Care transitions between outreach teams and clinics can fail silently if records are inconsistent. Simple unified forms and checklists dramatically improve continuity and reduce missed interventions.
Early childhood development benefits from integrated screening and caregiver coaching. Families respond well when guidance includes play, communication, and nutrition in one coherent framework.
Implementation Components
Component 1: Design a life-course care pathway with clearly defined touchpoints: antenatal registration, birth preparedness, facility delivery linkage, postnatal follow-up, immunization adherence, and developmental screening.
This component is implemented through a weekly rhythm that includes community engagement, service delivery alignment, and follow-up verification. Teams assign accountable owners, set timelines, and track completion so activities are not left at awareness level alone.
Component 2: Use household-level care plans that identify risk factors early, including anemia history, prior obstetric complications, and nutrition vulnerability. Risk plans should trigger proactive follow-up rather than reactive escalation.
This component is implemented through a weekly rhythm that includes community engagement, service delivery alignment, and follow-up verification. Teams assign accountable owners, set timelines, and track completion so activities are not left at awareness level alone.
Component 3: Introduce mother circles led by trained facilitators where participants exchange practical coping strategies and receive verified guidance from health workers.
This component is implemented through a weekly rhythm that includes community engagement, service delivery alignment, and follow-up verification. Teams assign accountable owners, set timelines, and track completion so activities are not left at awareness level alone.
Component 4: Integrate breastfeeding support, maternal mental health check-ins, and newborn danger-sign education into one postnatal workflow to reduce fragmentation.
This component is implemented through a weekly rhythm that includes community engagement, service delivery alignment, and follow-up verification. Teams assign accountable owners, set timelines, and track completion so activities are not left at awareness level alone.
Component 5: Implement child growth and development dashboards at community level so volunteers can quickly identify children needing additional support.
This component is implemented through a weekly rhythm that includes community engagement, service delivery alignment, and follow-up verification. Teams assign accountable owners, set timelines, and track completion so activities are not left at awareness level alone.
Component 6: Build referral and back-referral routines where facilities notify community teams after each critical visit, allowing continuity support at home.
This component is implemented through a weekly rhythm that includes community engagement, service delivery alignment, and follow-up verification. Teams assign accountable owners, set timelines, and track completion so activities are not left at awareness level alone.
Three-Phase Delivery Roadmap
Phase 1: Foundation and Trust Building. Teams recruit and orient local champions, validate referral pathways with partner facilities, and establish clear communication channels. During this period, health education emphasizes relevance and practical actions instead of broad messaging.
Phase 2: Integrated Service Delivery. Outreach events shift from awareness-heavy gatherings to structured preventive workflows. Screening, counseling, referrals, and follow-up enrollment happen as one sequence. Data quality checks are conducted weekly to prevent record drift.
Phase 3: Continuity and Scale. Teams analyze patterns in missed referrals, late follow-up, and recurring risk profiles. Lessons are translated into refined protocols, then expanded through adjacent communities using trained peer implementers and local government collaboration.
Monitoring, Learning, and Accountability
Effective community health work depends on disciplined measurement. Kenford Trust tracks process and outcome indicators together so program teams can see both activity volume and real behavior change. Process metrics include session attendance, screening completion, and referral issuance. Outcome metrics include referral completion, repeat preventive visits, and early risk detection trends.
Monthly learning reviews are essential. During these reviews, teams identify which cohorts are improving and which are falling behind. Corrective action plans are then documented with named owners and deadlines. This prevents common implementation failure where problems are discussed but not resolved.
Program accountability also includes community feedback loops. Participants should have clear channels to report concerns about service quality, communication clarity, and accessibility constraints. Transparent response to feedback builds trust and improves retention in prevention pathways.
To protect delivery quality, field supervisors run structured spot checks that evaluate communication clarity, referral accuracy, wait-time management, and participant experience from first contact to follow-up confirmation. These checks create practical learning moments for outreach teams and prevent drift from established service standards.
Field Execution Notes From Ongoing Community Work
Field Note 1: Expectant mothers frequently report that the first clinic visit feels manageable, but repeat visits become difficult as transport costs rise and family responsibilities increase. Continuity planning must therefore include social and economic realities from the beginning. In implementation, teams convert this context into a simple action chain: identify affected households, align outreach timing with local routines, provide risk-specific prevention guidance, and confirm referral completion within a defined time window. This approach keeps interventions practical and measurable while preserving dignity in every interaction.
Field Note 2: Community birth companions often understand household dynamics better than formal providers. When they are linked to facility teams through a clear referral protocol, women receive more consistent encouragement to complete antenatal pathways. In implementation, teams convert this context into a simple action chain: identify affected households, align outreach timing with local routines, provide risk-specific prevention guidance, and confirm referral completion within a defined time window. This approach keeps interventions practical and measurable while preserving dignity in every interaction.
Field Note 3: In many communities, fathers are willing to support maternal health but lack practical information. Structured father-inclusive sessions can transform passive support into concrete actions such as transport planning and postnatal monitoring. In implementation, teams convert this context into a simple action chain: identify affected households, align outreach timing with local routines, provide risk-specific prevention guidance, and confirm referral completion within a defined time window. This approach keeps interventions practical and measurable while preserving dignity in every interaction.
Field Note 4: Postnatal care is commonly misunderstood as optional when the delivery appears uncomplicated. Outreach messaging must explain why postpartum checks are essential for both mother and child, even in seemingly stable cases. In implementation, teams convert this context into a simple action chain: identify affected households, align outreach timing with local routines, provide risk-specific prevention guidance, and confirm referral completion within a defined time window. This approach keeps interventions practical and measurable while preserving dignity in every interaction.
Field Note 5: Caregivers of newborns often navigate conflicting advice from relatives, social media, and neighbors. Trusted local educators can reduce confusion by offering consistent guidance anchored in evidence and practical examples. In implementation, teams convert this context into a simple action chain: identify affected households, align outreach timing with local routines, provide risk-specific prevention guidance, and confirm referral completion within a defined time window. This approach keeps interventions practical and measurable while preserving dignity in every interaction.
Field Note 6: Nutrition counseling is more effective when linked to local food availability and household purchasing patterns. Generic recommendations rarely translate into action without adaptation to community context. In implementation, teams convert this context into a simple action chain: identify affected households, align outreach timing with local routines, provide risk-specific prevention guidance, and confirm referral completion within a defined time window. This approach keeps interventions practical and measurable while preserving dignity in every interaction.
Field Note 7: Care transitions between outreach teams and clinics can fail silently if records are inconsistent. Simple unified forms and checklists dramatically improve continuity and reduce missed interventions. In implementation, teams convert this context into a simple action chain: identify affected households, align outreach timing with local routines, provide risk-specific prevention guidance, and confirm referral completion within a defined time window. This approach keeps interventions practical and measurable while preserving dignity in every interaction.
Field Note 8: Early childhood development benefits from integrated screening and caregiver coaching. Families respond well when guidance includes play, communication, and nutrition in one coherent framework. In implementation, teams convert this context into a simple action chain: identify affected households, align outreach timing with local routines, provide risk-specific prevention guidance, and confirm referral completion within a defined time window. This approach keeps interventions practical and measurable while preserving dignity in every interaction.
Partnership and Sustainability Architecture
Long-term health impact requires partnerships that are specific, accountable, and operationally clear. Kenford Trust coordinates with county health teams, facility managers, local schools, faith communities, and community-based organizations so responsibilities are explicit and duplication is minimized. Clear role definitions allow each partner to contribute where they are strongest while preserving a unified pathway for community members.
Sustainability improves when capacity building is embedded in routine delivery. Rather than relying on occasional workshops, teams run continuous coaching that strengthens referral documentation, communication quality, and case prioritization. As local actors gain confidence and consistency, programs become less dependent on external supervision and more resilient during funding or staffing fluctuations.
Financial sustainability also depends on practical design. Outreach plans prioritize low-cost, high-frequency actions that can be maintained by local teams. Where additional resources are needed, data-backed evidence on outcomes helps partners mobilize support from aligned institutions and responsible donors.
Operational sustainability: local ownership of planning, delivery, and follow-up routines.
Financial sustainability: cost-aware models with transparent budgeting and measurable returns.
Institutional sustainability: shared protocols that survive leadership transitions.
Risk Management and Mitigation
Every community health program faces implementation risks, including volunteer fatigue, referral bottlenecks, misinformation spikes, and data inconsistency. Kenford Trust addresses these risks through preventive controls: rotating workloads, escalation pathways with facilities, rumor response protocols, and weekly data audits.
Another common risk is uneven service quality between neighborhoods. To address this, teams standardize core workflows while allowing contextual adaptation in language, scheduling, and session format. Standardization protects quality; adaptation protects relevance.
Privacy and confidentiality are treated as non-negotiable safeguards. Teams receive practical guidance on consent, secure documentation, and respectful communication, especially in sensitive cases involving mental wellbeing, maternal health concerns, and chronic disease management.
Finally, mitigation plans are documented before scale expansion. If a new site cannot sustain referral follow-up, data quality, and community trust thresholds, expansion is paused until foundational gaps are closed.
Expected Impact Trajectory
Higher completion rates for antenatal and postnatal visits through clearer care pathways and community-based follow-up.
Earlier identification of maternal and neonatal risks, enabling faster response and better clinical outcomes.
Stronger caregiver confidence in newborn care practices, feeding decisions, and danger-sign recognition.
Reduced dropout across immunization and growth monitoring schedules in the first two years of life.
Improved family-level understanding of preventive care as a continuous process rather than a one-time event.
A replicable continuity model suitable for expansion through county partnerships and community networks.
Over time, the practical value of this model is not only improved statistics but also improved confidence. Families begin to see preventive care as routine, not exceptional. Local volunteers become capable navigators instead of passive messengers. Facilities gain better continuity data and can prioritize high-risk cases more effectively.
Kenford Trust remains committed to health systems that protect dignity while improving outcomes. Every outreach strategy is therefore judged by a core question: does this approach make it easier for people to sustain healthy behavior over time? If the answer is no, we redesign it. If the answer is yes, we strengthen and scale it with partners.
External Learning Links
Community health succeeds when prevention becomes ordinary, trusted, and locally owned.